Breastfeeding or Formula Feeding: Which one is ideal for your Baby?
Are you a new mom? Juggling between overwhelming pieces of advice about how to feed a baby?
What is good for my infant? Is formula good for my baby?
For how long do I have to breastfeed?
Whether stored breast milk is good or not?
My baby is hungry after my feed? Will Formula help?
Take a DEEP BREATH!
You are not alone, almost every new mother feels doubtful, vulnerable, and confused and wants a handhold from an expert to help her navigate the early motherhood challenges from hospital to home.
I am super grateful that I do the same work as a Lactation Consultant and support new families with exclusive breastfeeding starting from their hospital-to-home journey.
Daily, I meet so many new moms and listen to their struggles patiently, every story is different, and yet it sounds the same.
I feel blessed to support new mothers by empowering them to confidently breastfeed their babies from day one
Today I am sharing a beautiful story of a new mother who made an informed choice between Breast milk and Formula with our loving, non judgemental consistent support and experience of empowerment
A new mom who had a c-section delivery with a three-day-old baby called me for a home visit in Gurugram. I was super ready with my notes for mother and baby assessments, with my dummy models to show the ideal positionings and latch techniques accurately to the new, worried mother who was desperate to learn to breastfeed joyously.
The breastfeeding dyad (new mother, new father, new baby) had a goal of feeding exclusively for two years. Unfortunately, alternative feeding(formula) has taken all the space as the primary source of nutrition for the baby. They had no idea how to turn around and breastfeed exclusively, as the baby was not put at the mother’s breasts and not fed frequently on his hunger cues.
When I finally met the mom, I was shocked to see how the baby was unknowingly fed formula every two hrs. New parents were never guided to make an informed choice before or after the birth of a child. No surprise the mother was not producing enough milk to satisfy the baby.
My ultimate goal was to support the new mother and baby with ideal positions and latch techniques so that the baby begins the effective milk removal every two hrs, fed on hunger cues with skin-to-skin done by the new parents.
A new adorable little one did a fantastic job at the first attempt when he was well supported on his mother’s breasts. He effectively suckled colostrum for a good 45-50 minutes from both breasts and slept as a milk drunk.
I was successful in supporting the mother and baby, I blessed them and left home..
No, I wasn’t successful at the root level..soon I realized. There was a miss!
My work is not only to guide on positions or latches and help them to heal sore nipples.
Instead, my work is to support the new parents to make informed choices antenatally, postnatally, and at the time of weaning, supporting them to lay the foundation of love (for self), freedom(from chaos), and the highest level of well-being of the child.
By the time, I reached home, I was clear and ready to pen my thoughts to support all new mothers and fathers, supporting them to understand what is the real difference between Breastmilk and Formula milk: for the benefit of all!
I am sure you will be well informed by the end of this article and will always make informed choices and support other new parents too.
How does Breast Milk develop prenatally?
Prenatally, hormonal changes influence the breast changes, which stimulate ductal sprouting and are involved in the final preparation of the glandular tissues for copious milk production
(another name is Lactogenesis 1 or L1) That means milk occurs at the 16th prenatal week. So, it is there already and never short for a baby. Effective milk removal has to happen with expert lactation support.rt
When copious milk production happens, (called Lactogenesis 2 or L2) the mother feels fullness around 50-72 hrs after birth and should feed the baby within 1 hrs of birth.
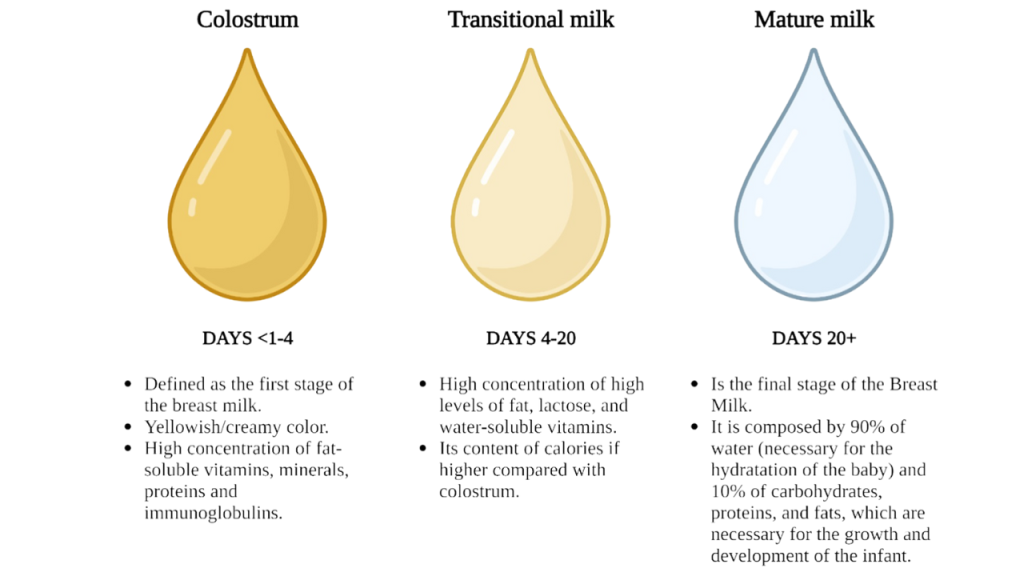
Why Exclusive Breast Milk Acts as Gold Liquid?
It has countless benefits.
Micronutrients in breast milk provide energy for the infant and help in growth in development. The energy provided by the breastmilk is 60-70 kcal/ 100 ml of breastmilk. Every drop is GOLD.
Breast Milk has the majority of water, that’s why no additional water is required for the first six months of life even in hot or dry climates.
Human milk contains more than 200 fatty acid structures, providing infants with caloric requirements contributing to 30-40 % of the total fatty acids. Interestingly, fats are most variable in human milk and increase during feeding and as the child grows older. They are generally based on maternal diet.
Also, fat content in human milk increases and is 8 times higher after the baby feeds when the breasts are softened. Tell me, would you miss feeding your baby?
Human milk contains more than 400 different proteins that provide calories, immune factors, growth factors, hormones, and enzymes needed for a baby’s growth and development. Colostrum has a high protein concentration during the first few days of lactation.
Human milk contains Lactoferrin, which suppresses E.coli in the intestine. It facilitates iron absorption and stimulates intestinal epithelial cell growth.
Carbohydrates in human milk serve as prebiotics, providing energy to the beneficial bacteria inside the infant’s intestine.
Beneficial bacteria protect the infant from disease-causing bacteria that cause diarrhea and respiratory infections. Carbohydrates (HMO) protect infants from viruses, bacteria, and protozoa and strengthen immune cells.
Human milk contains an adequate amount of vitamins needed for infant growth, except Vitamin D and K. That is why the amount of vitamin D depends on the diet and maternal sun exposure
Interesting Fact,
Frozen breastmilk retains most anti-infective properties and is nutritionally superior to Formula.
What should Breastfeeding Moms know about Formula Feeding?

Parents consider giving their babies formula(as my new mother gave, believing she has a low milk supply, even when the milk supply was fine) for many reasons. In some cases, it’s medically necessary. Sometimes it’s simply the parents’ choice.
Keep in mind that formula (like a medicine) comes with its own set of risks, and parents need to be aware of these so that they can make an informed decision on its use.
The use of formula can shorten the breastfeeding relationship and come with increased health risks for the baby and the mother.
Remember, breastfeeding does not have to be, ‘ all or nothing’. Any amount of breastmilk is beneficial to both mother and baby.
What are The Risks of Not Breastfeeding for Mothers and Infants?
For infants, not being fed human milk is associated with an increased risk of morbidity, including Otis Media, gastroenteritis, pneumonia, and elevated risk of type 1 and type 2 diabetes and SIDS.
- NecrotizingEnterocolitis NEC,
- Lower respiratory tract infection,
- Obesity,
- Slow cognitive development,
- Asthma,
- Atopic dermatitis,
- Childhood cancer,
For mothers, failure to breastfeed is associated with an increased incidence of premenopausal breast cancer, ovarian cancer, retained gestational weight gain, type 2 diabetes, and metabolic syndrome.
Role of a medical health professional: counseling during antenatal sessions. At Deliver Delights we do monthly sessions on breastfeeding awareness and guide our pregnant and lactating moms antenatally.
When the supplementation can be considered
- When a baby has asymptomatic hypoglycemia or baby has dehydration(>10% weight loss, poor feeding, and lethargy)
- When a baby has weight loss greater than 8% with delayed onset of milk increasing in volume( 5 days)
- When baby lacks in passing bowel movements or meconium stools on day 5
- When the baby doesn’t take sufficient intake despite an adequate milk supply
- When a baby is jaundiced has galactosemia or a baby who is unable to feed at the breasts and has congenital malformations.
- When a mother has primary lactation failure
My take-home message:
The strong feelings struck me for the new parents and their vulnerability.
The formula is sometimes medically necessary, but surely not when a mother feels there is a low milk supply, gets tired, or is simply under pressure. Evidence suggests that breastmilk has long-term health benefits for both mother and baby.
My previous blog would help you to deep dive and make an informed choice.
I believe that long-term health risks associated with formula feeding should be discussed frequently with parents to enable fully informed choices. It is also the responsibility of health professionals to make parents aware that formula feeding can potentially impact their child’s metabolic and immune systems and affect the child’s neurodevelopment.
In my opinion, I wholeheartedly agree that Formula dabbas should not be a luxury item to be placed in mothers’ rooms and allow them to room- in with their babies and learn breastfeeding with the support of skilled lactation consultants like us.
What do you think?
Love
Deepti.







